 Nordi Medical
Nordi Medical
 Nordi Medical
Nordi Medical
Hydrocolloid dressings have emerged as a pivotal component in burn treatment protocols. These advanced dressings offer both clinical and practical advantages. According to a report by the World Health Organization, appropriate burn management can significantly reduce healing time and the risk of infection. The question arises: "What are the benefits of using hydrocolloid dressings on burns?" Experts in the field, such as Dr. Emily Carter, emphasize that these dressings “promote a moist wound environment, vital for optimal healing.”
The use of hydrocolloid dressings minimizes pain associated with dressing changes. They conform to the wound, providing a protective barrier against external contaminants. Research indicates that patients experiencing burns treated with hydrocolloid dressings report lower pain levels during rehabilitation. This enhancement in patient comfort is crucial for psychological recovery, which is often overlooked in burn treatment.
Moreover, hydrocolloid dressings are easy to apply and can remain in place for extended periods. This reduces the frequency of dressing changes, allowing healthcare professionals to focus on other critical aspects of patient care. However, the cost-effectiveness of hydrocolloid dressings remains an area for further reflection. Balancing cost with clinical benefits is essential in ensuring equitable access to these innovative treatments for all patients.
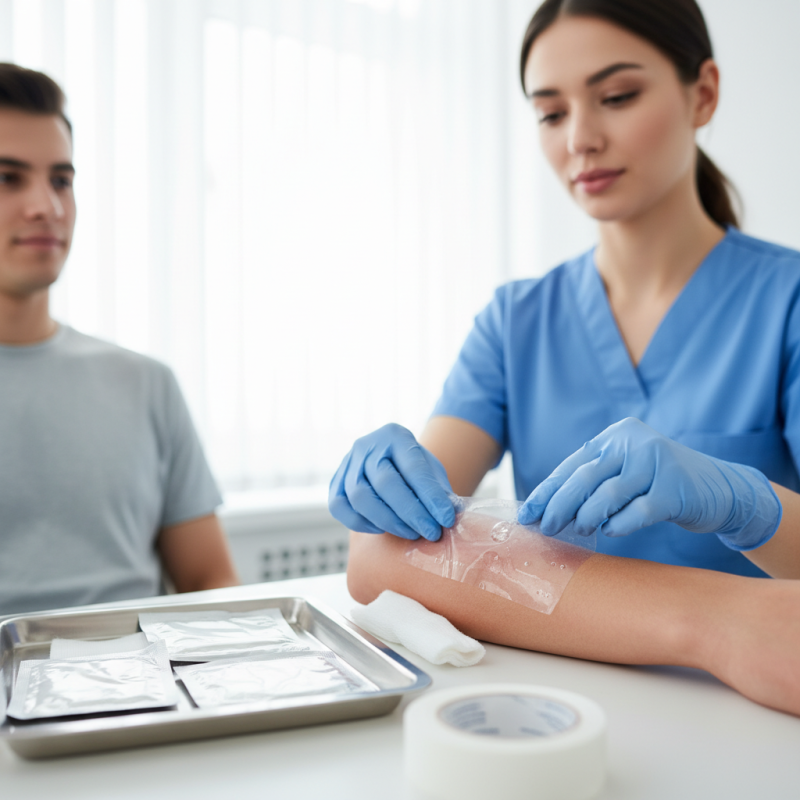
Hydrocolloid dressings are a popular choice in burn treatment due to their unique properties. They consist of gel-forming agents, such as pectin and carboxymethyl cellulose, combined with a semipermeable membrane. This composition allows them to absorb exudate while maintaining a moist environment around the wound. This environment promotes faster healing and minimizes pain during dressing changes.
The structure of these dressings is quite fascinating. When applied, hydrocolloid dressings adhere to the skin, creating a protective barrier against bacteria. They prevent contamination and reduce the risk of infection, which is crucial for burn patients. However, it's essential to monitor the dressing regularly. Sometimes, they may loosen or peel off prematurely, requiring timely replacement. Their ability to provide pain relief adds to their overall effectiveness.
While hydrocolloid dressings have many benefits, they are not without their challenges. Improper application can lead to complications, such as maceration of the surrounding skin. Healthcare providers need to be trained in their use to maximize effectiveness. Observing the healing process is vital. It's an ongoing journey, and adjustments may be necessary to ensure optimal care.
Hydrocolloid dressings are increasingly popular in burn treatment due to their unique mechanisms. These dressings contain a gel-forming agent that helps to create a moist environment. This environment not only promotes healing but also minimizes pain during dressing changes.
Clinical studies suggest that hydrocolloid dressings can reduce healing time by 20-30% in superficial burn cases. They protect the wound from infection and external contaminants while allowing excess moisture to escape. This balance aids in reducing the risk of maceration, which can complicate healing. Furthermore, patients often report less discomfort compared to traditional dressings.
Tip: Regularly monitor the dressing for signs of saturation or detachment. Change it as needed to maintain cleanliness and moisture balance.
The effectiveness of hydrocolloid dressings is linked to their adhesive properties, promoting secure placement. However, it's essential to consider individual skin sensitivities. Some patients may experience irritation, indicating a need for alternative options. Health practitioners should assess each case carefully to ensure optimal outcomes.
Hydrocolloid dressings are an innovative solution for treating burns. The chart above illustrates various benefits, including faster wound healing speed, significant pain reduction, effective infection control, enhanced patient comfort, and minimized scarring, demonstrating their importance in burn treatment strategies.
Hydrocolloid dressings offer significant advantages over traditional dressings in burn treatment. They create a moist environment that promotes healing. This moisture helps reduce pain and speeds up recovery time. Unlike traditional bandages, hydrocolloid dressings adhere to the skin without sticking to the wound, minimizing trauma when changing them.
Tips: Keep the dressing clean and dry to maintain its adhesive properties. Change it as recommended by a healthcare professional. Monitor the burn for signs of infection, such as increased redness or swelling.
The flexibility of hydrocolloid dressings allows for movement without disrupting the wound. They are also water-resistant, providing added protection against bath and shower exposure. In contrast, traditional dressings can become soggy and lose their efficacy quickly.
Tips: If using hydrocolloid dressings for larger burns, consider consulting a specialist for personalized advice. It's essential to have realistic expectations about healing times. Each burn is unique, and reactions may vary.
Hydrocolloid dressings have gained attention in burn treatment. Clinical studies demonstrate their effectiveness and healing properties. These dressings maintain a moist environment, which promotes faster healing of burns. Moisture can reduce pain and the risk of infection.
Research indicates that patients using hydrocolloid dressings experience less discomfort than those with traditional dressings. These dressings adhere well to the skin, minimizing the chances of peeling and disruption. Compression is vital for healing, and hydrocolloids provide this without causing additional trauma.
Despite these benefits, some challenges remain. Not all burns may respond to hydrocolloid dressings. Skin reactions can occur, leading to discomfort in some patients. Proper assessment by healthcare professionals is essential to determine suitability. This approach ensures the use of hydrocolloid dressings aligns with individual patient needs.
| Benefit | Description | Clinical Evidence |
|---|---|---|
| Moist Healing Environment | Hydrocolloid dressings create a moist environment that promotes faster healing. | Studies show reduced healing time compared to traditional dry dressings. |
| Reduced Pain | These dressings can minimize pain during dressing changes. | Clinical trials indicate lower pain scores with hydrocolloid use. |
| Protection from Infection | Hydrocolloid dressings provide a barrier against bacteria. | Research shows decreased infection rates in burn wounds covered with hydrocolloids. |
| Ease of Use | These dressings are easy to apply, adjust, and remove. | Surveys show positive feedback from healthcare providers on usability. |
| Cost-Effectiveness | Hydrocolloids can reduce the overall cost of burn treatment. | Economical analyses suggest lower costs due to reduced healing time and fewer complications. |
Hydrocolloid dressings are effective for burn treatment due to their moisture-retentive properties. When applied correctly, they provide a protective barrier against bacteria. This reduces the risk of infection. They also promote healing by keeping the wound moist, which can minimize pain and scarring.
Applying hydrocolloid dressings requires careful preparation. Clean the burn area gently with mild soap and water. Pat it dry with a clean cloth, avoiding any friction. Choose a dressing that adequately covers the burn size. Ensure the edges adhere well to the skin. Do not stretch the dressing as this can cause discomfort.
Monitoring the dressing is crucial. Change it if it becomes saturated or loose. If you notice any signs of infection, such as increased redness or pus, seek medical advice promptly. While hydrocolloid dressings are effective, they may not be suitable for all types of burns. Always assess the burn and consider consulting a healthcare professional for personalized guidance.
: They contain gel-forming agents like pectin and carboxymethyl cellulose. They also have a semipermeable membrane.
They absorb exudate and maintain a moist environment, promoting faster healing and less pain during changes.
They create a barrier against bacteria and reduce infection risks. This is crucial for patients with burns.
Yes, they may loosen or peel off prematurely, requiring careful monitoring and timely replacement.
Improper application can lead to skin maceration. Training for healthcare providers is essential to avoid complications.
Patients report less discomfort with hydrocolloid dressings. They adhere better and reduce disruption during the healing process.
Yes, some burns may not respond well. Proper assessment is necessary to ensure suitability for each patient.
The healing process should be observed closely. Adjustments may be needed to ensure optimal care and outcomes.
Yes, skin reactions can occur, leading to discomfort in some patients. This highlights the need for individual assessment.
Compression is vital. Hydrocolloid dressings provide it without causing additional trauma to the healing skin.
Hydrocolloid dressings represent an innovative approach in burn treatment, offering numerous benefits that enhance healing and patient comfort. These dressings are composed of gel-forming agents that maintain a moist environment, crucial for optimal wound healing. The mechanism of action involves absorption of exudate while allowing gaseous exchange, which helps prevent infection and promotes faster recovery.
What are the benefits of using hydrocolloid dressings on burns? These dressings are easier to apply and remove compared to traditional methods, minimizing pain and trauma during dressing changes. Clinical evidence supports their effectiveness, indicating reduced healing times and less scarring. Additionally, hydrocolloid dressings provide a protective barrier that aids in pain management. For best results, proper application techniques are essential, ensuring that the dressing adheres well to the skin and adequately covers the burn area.
